Anal canal cancer
Eighty percent of anal cancers are squamous cell carcinomas (SCCs). Other tumour types include melanoma, lymphoma and adenocarcinoma. The behaviour of the tumour depends on the anatomical site of the primary cancer.
The anal canal extends from the anorectal junction to the anal margin. The dentate line marks the junction between the squamous and mucosal epithelium in the anal canal. Immediately above the dentate line, there is a zone of transitional epithelium. Below the dentate line, the canal is lined by non-keratinising squamous epithelium, which merges with the perianal skin. The anal margin is the pigmented skin immediately surrounding the anal orifice.
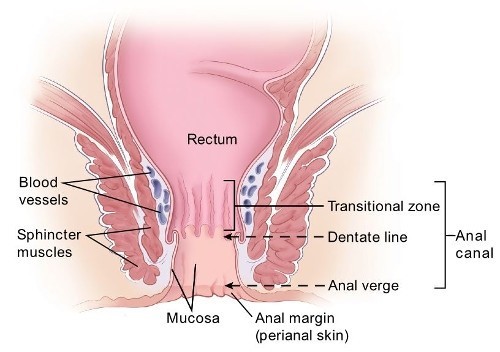
The lymphatic drainage varies in different parts of the canal. The drainage is close in proximity to the perirectal nodes along the inferior mesenteric artery. The lymph that is located immediately above the dentate line drains to the internal pudendal nodes and then to the internal iliac system. The infra-dentate and perianal skin drains to the inguinal, femoral and external iliac nodes.
Epidemiology
Anal cancer is an uncommon malignancy. It accounts for only about 4 percent of all cancers of the lower alimentary tract. Anal cancer occurs in about 1 in 100,000 people. However, it is more common in women and is increasing.
Anal margin tumours: These tumours are usually well differentiated. They are more common in men and have a good prognosis.
Anal canal tumours: These tumours are usually poorly differentiated. They are more common in women and have a poor prognosis. Systemic spread of anal cancer occurs in fewer than 10 percent of cases. It spreads most commonly to the liver and lungs.
Risk Factors
Human papillomavirus (HPV) is an important aetiological factor and 50 percent of tumours contain viral DNA. Anal intercourse and a multiple sexual partners increase the risk of HPV infection. Anal carcinoma is more common in men who have sex with men. People who have HIV infection and patients who take immunosuppressive drugs for HIV infection are more susceptible to anal carcinoma. It is twice as common in HIV-positive men as it is in HIV-negative men who have sex with men.
Other important risk factors include immune suppression in transplant recipients and cigarette smoking. Previous malignancy (e.g., gynaecological, lymphoma or leukaemia) or subsequent malignancy (e.g., lung, bladder, vulva, vagina or breast) is more likely in patients with anal cancer.
Presentation
Presentation includes perianal pain and bleeding, a palpable lesion and faecal incontinence. Neglected tumours in women can cause a rectovaginal fistula. Tumours near the anal margin spread to the inguinal lymph nodes. Those higher in the anal canal spread to the pelvic lymph nodes.
Investigations
A biopsy should always be conducted for suspicious lesions. Rectal examination under anaesthesia and biopsy are the most useful staging investigations. Imaging modalities used for staging include CT, MRI, endo-anal ultrasound and positron emission tomography (PET). Patients should be tested for relevant infections, including HIV and other possible malignancies.
Staging
The American Joint Committee on Cancer and the International Union Against Cancer have described a staging system for anal canal cancer. Tumours of the anal margin (below the anal verge and involving the perianal hair-bearing skin) are classified as skin tumours.
Primary tumour (T): TX: Primary tumour cannot be assessed.T0: No evidence of primary tumour. Tis: Carcinoma in situ. T1: Tumour is 2 cm or less in greatest dimension. T2: Tumour is more than 2 cm but not more than 5 cm in greatest dimension. T3: Tumour is more than 5 cm in greatest dimension. T4: Tumour is of any size that invades adjacent organ(s) (e.g., vagina, urethra, bladder [direct invasion of the rectal wall, perirectal skin, subcutaneous tissue, or the sphincter muscle(s)] is not classified as T4).
Regional lymph nodes (N): NX: Regional lymph nodes cannot be assessed. N0: No regional lymph node metastasis. N1: Metastasis is in perirectal lymph node(s). N2: Metastasis is in unilateral internal iliac and/or inguinal lymph node(s). N3: Metastasis is in perirectal and inguinal lymph nodes and/or bilateral internal iliac and/or inguinal lymph nodes.
Distant metastasis (M):
MX: Distant metastasis cannot be assessed. M0: No distant metastasis. M1: Distant metastasis.
Stage groupings
Stage 0: Tis, N0, M0. Stage I: T1, N0, M0. Stage II: T2, N0, M0; T3, N0, M0.
Stage III A: T1, N1, M0; T2, N1, M0; T3, N1, M0; T4, N0, M0.
Stage III B: T4, N1, M0; any T, N2, M0; any T, N3, M0.
Stage IV: any T, any N, M1.
Management
Local excision can be considered for small well-differentiated carcinomas of the anal margin. The recommended first-line treatment is combined modality chemotherapy and radiotherapy using 5-fluorouracil and mitomycin C. Salvage surgery is reserved for more severe cases of carcinomas.
For all stages of localised SCC of the anal canal, concurrent chemotherapy and radiotherapy are recommended over radiotherapy alone to improve local control and decrease colostomy rates. The optimal chemotherapy combination for SCC of the anal canal is 5-fluorouracil plus mitomycin C given concurrently with radiation treatment.
The addition of chemotherapy allows lower radiation doses to be used. Therefore, the effects are less toxic. Combination chemoradiotherapy is considered the treatment of choice for adenocarcinoma as well as SCC.
Radiotherapy
Radiotherapy is given to the tumour and inguinal nodes. Radiation therapy alone may lead to a 5-year survival rate in excess of 70 percent. However, high doses may be required and cause necrosis or fibrosis.
Chemotherapy
Chemotherapy concurrent with lower-dose radiation therapy has a 5-year survival rate in excess of 70 percent, with low levels of acute and chronic morbidity. Few patients may need surgery for toxic effects (such as anal stenosis or anal necrosis). Radiation with continuous infusion of fluorouracil plus cisplatin is also under evaluation. However, the role of cisplatin in anal cancer is not currently clear.
Metastatic disease is less responsive to combined chemotherapy and radiation treatment. HIV patients with pretreatment CD4 counts of fewer than 200 cells/mm3 may have increased acute and late toxic effects. Doses of radiation and chemotherapy drugs may need to be modified.
Surgery
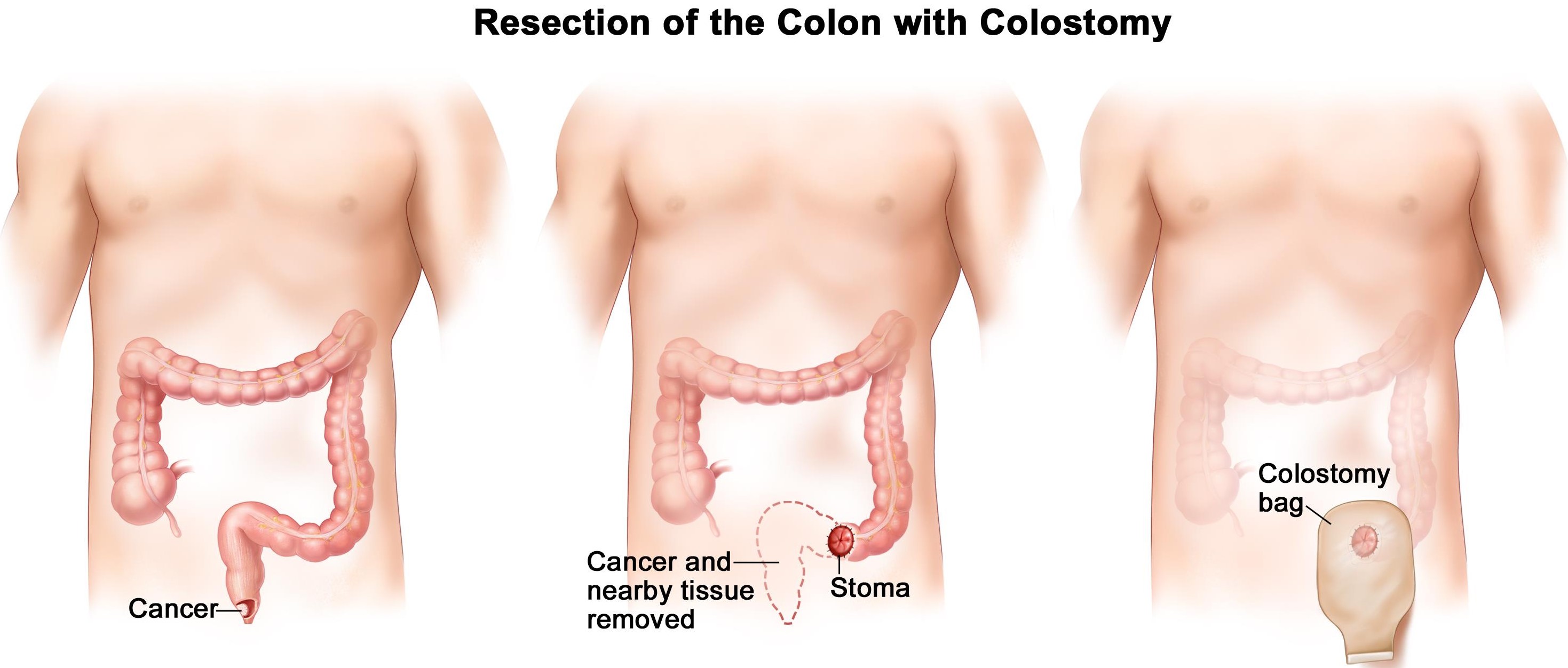
Surgery is required for the following:
• Tumours that fail to respond to radiotherapy.
• Large tumours that cause gastrointestinal obstruction.
• Small anal margin tumours without sphincter involvement.
Standard salvage therapy for patients with residual disease following chemoradiotherapy has been abdominoperineal resection. Alternatively, patients may be treated with additional salvage chemoradiotherapy in the form of fluorouracil, cisplatin and a radiation boost to potentially avoid permanent colostomy.
Patients with anal cancer may require radical inguinal lymphadenectomy.
Complications:
Complications of radiation therapy include anal ulcers, anal stenosis and necrosis.
Prognosis
The overall 5-year survival rate was 62 percent in 1980s. It has changed little in a period of two decades. The reported 5-year survival rate following surgery is 40–70 percent. The three major prognostic factors are site, size and lymph node status. Anal margin tumours are better differentiated and have a better prognosis than anal canal tumours
A cutoff of 4–5 cm has been proposed as the size that distinguishes good and poor prognosis. The level of tumour regression (>80 percent) after primary chemoradiation may be predictive of colostomy-free survival and disease-free survival. Radiation therapy, given as external-beam or brachytherapy, has a cure rate of 70–90 percent in selected patients. The cure rate is about 50 percent for people with tumours larger than 5 cm or if lymph nodes are involved.